What is a Pressure Ulcer?
A pressure ulcer is damage to the skin and the deeper layer of tissue under the skin. It can also be referred to as a pressure sore or bed sore.
If pressure is applied over a long period of time, particularly over a bony area of your body, such as your ears, heels, sacral area or spine, the skin and muscles can be damaged. This damage can show on your skin, or can occur deeper in your body and work its way out to your skin.
Causes
Pressure ulcers are commonly caused by sitting or lying in one position for too long without moving. This is more likely to happen when you are feeling unwell, and/or you are experiencing pain, discomfort or tiredness, which is affecting your ability to change position regularly.
For this reason, pressure ulcers can be very difficult to heal and treat. Without care, they can become very serious, resulting in increased pain as well as an increased risk of infection, which can lead to Sepsis.
Prevention is the key
- Keeping moving. Change position 2-4 hourly. This could be a big change such as turning in bed from the left side to the right, or a smaller turn such as using bed controls to alter the position of the headrest or knee raise.
- Use pressure relieving equipment provided. Air mattresses and chair cushions are medical devices that will support your pressure area care needs.
- Take care of your skin by keeping it clean and dry. Water based moisturisers can also help.
- Eat well and keep hydrated if you can.
- Tell your nursing team if you experience any changes in the condition of your skin, or discomfort over a bony prominence.
Warning!
Early warning signs
An early warning sign to look out for is a change in the colour of the skin – a patch of skin may be red, which occurs more with pale skin, or a patch of skin may become discoloured and turn purple or blue, which tends to happen with darker skin.
To check whether a change in skin colour is the early stages of a pressure ulcer, you can apply light finger pressure to see if it turns white. A pressure ulcer will not change colour.
Categories of Pressure ulcer
Pressure ulcers fall into one of four stages depending on their depth, severity, and physical characteristics.
Category 1
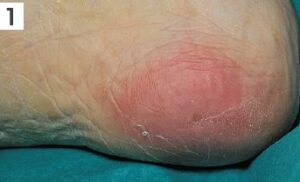
The skin is still intact and the area may be painful, firm, soft, warmer or cooler compared to the tissue alongside it.
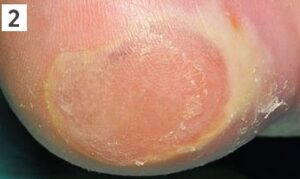
Category 2
The area continues to break down and becomes an open shallow wound. This can happen rapidly without movement.
Category 3
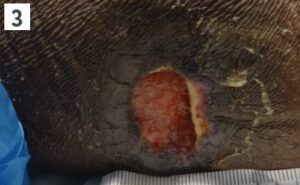
A deeper wound that affects all the layers of skin. Subcutaneous fat may be visible, but bone, tendon or muscle are not exposed.
Category 4
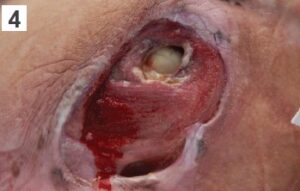
A much deeper wound with full tissue loss and bone, tissue or muscle exposed.
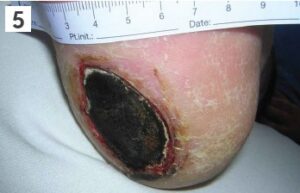
Category 5
You may hear nursing staff refer to an unstageable pressure ulcer. This is when an area of skin has become dark purple or black in colour.
How we can support you
Nursing staff will discuss how to monitor your
skin areas with you, so that a plan can be put in place to protect your pressure areas. Should a pressure ulcer develop, a member of the nursing team will advise on creams, dressings and pressure area care. In the community, a referral to the district nursing will be completed.
Caring for pressure areas for people who are nearing the end of life
Pressure ulcer development is a higher risk at this time as people don’t tend to be able to move or change position as regularly, and may lose ability to control bowel or bladder movements, which can cause damage and discomfort. If a pressure ulcer occurs then the focus of care will be on ensuring comfort, rather than healing the area.
Making a decision on pressure area care
The nursing team will talk to you about the importance of regular pressure area care to reduce the risk of pressure damage which can grow and become deeper, becoming, more painful and malodourous (smelly).
The team will ensure that you understand the implications of not receiving this care, meaning a pressure damage could develop or become significantly worse.
For some people the pain from a pressure ulcer can cause more discomfort than the symptoms of their condition.
Care, particularly at the end of life, can be a balance between comfort and prevention of possible complications. The team will ensure that you have all the necessary information to make an informed decision and support your right to do so. They will be happy to review this decision with you should you change your mind. They will document this discussion in the nursing notes and ensure care plans are updated accordingly.
Comments
We are always pleased to hear any comments about the services we are providing. Your feedback helps us to maintain a high standard of service and we are really keen to hear from you. You can also complete our feedback survey via our website. Please visit: www.farleighhospice.org/feedback
Useful Numbers:
General enquiries: 01245 457300
Inpatient Unit (IPU): 01245 457361
Advice Line: 01245 455478 (8am – 8pm)
